Macular degeneration
Macular degeneration – Written by Dr. Ali Dirani, MD, MSc, MPH and Mélanie Hébert, MD, MSc.
What is myopic macular degeneration?
In myopia or near-sightedness, there is elongation of the eye which stretches the retina (light sensitive tissue at the back of the eye) and this may lead to areas of fragility that are prone to break. When these areas break, it causes retinal tears or holes. The vitreous (transparent jelly that nourishes the eye and fills the eyeball) can then go behind the retina and detach it from the back of the eye causing a retinal detachment leading to vision loss.
Apart from causing fragility of the retina, myopia can also cause stretching of the macular (area of the retina that allows us to enjoy clear central vision and colour vision). The photoreceptors (cells at the macular responsible for vision) are fragile and stretching can cause macular atrophy (reduced number of cells) or reduced function due to thinning.
Along with the photoreceptor cells, the retinal pigment epithelium (RPE) provides vision and nutrition and is essential to the retina’s survival. Damage to these layers lead to myopic macular degeneration (MMD).
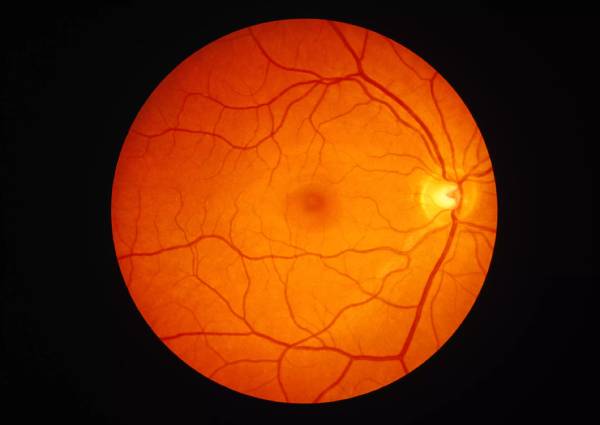
Figure 1 below illustrates the appearance of a healthy retina in an eye with no myopic macular degeneration. Figure 2 illustrates the gradual loss of the layers of the retina, with increasing severity. MMD progression is seen with the patches of paler, white areas which represent areas where much of the retina is lost.

The global problem of macular degeneration
Studies show that about 1.1 to 3.1% of people may have myopia macular degeneration [2]–[5]. Overall, this is about 2 in every 100 people worldwide [6]. People who have myopia are those at greatest risk for myopic macular degeneration, usually with a myopia greater than −6 dioptres (unit to measure the power of lens required to correct myopia).
Nearly 90% of people with myopia greater than −10 dioptres develop this condition [4]. The greater the severity of myopia, the more likely someone can have myopic macular degeneration and the more likely it will progress.
Older people are also more likely to develop this condition. Among patients with myopic macular degeneration, about half of them will have disease in both eyes and about a third of affected eyes have visual impairment (less than 20/40 on a vision chart) [3]. This may worsen with time though.
What are the common signs and symptoms of macular degeneration?
Depending on the complication of myopic macular degeneration, people can have multiple different signs and symptoms. With new retinal tears and holes, flashes of light or floaters may be noticed. When people have atrophy of the retina, posterior staphyloma, and lacquer cracks, these cause vision loss which cannot be corrected with eyeglasses. Choroidal neovascularisation (CNV), a complication of myopic macular degeneration causes vision loss as well but can also cause distortions of straight lines, a phenomenon called metamorphopsia.
If you experience any of these signs and symptoms, schedule an appointment with an eye health professional to get your eyes checked. It is also important to note that the development of eye conditions may even start before symptoms appear, which makes going for regular and timely eye checks that much more essential.
How is macular degeneration diagnosed?
People generally learn that they have myopia when they have their annual eye check-up with eye care professionals for the prescription of glasses if needed or when they notice trouble seeing at a distance.
When people notice flashes, floaters, vision loss or metamorphopsia (distortion of straight lines), an eye care professional will do a full eye exam, including a dilated fundus exam. This is when the pupil, which is the dark centre of the eye, is increased in size using eyedrops to better see the retina at the back of the eye.
The eye care professional could then shine light into your eye to see the back and could use different types of lenses to magnify the retina to better see it. Different types of instruments can be used to see the retina.

As seen in Figure 3 above, three-mirror lens can be used at the slit lamp which is the microscope that eye care professionals use to examine eyes. This is a contact lens that is placed on the eye to see the entire retina including the periphery. Eye drops are instilled to temporarily numb the surface of the eye before using this lens to make it more comfortable.

As seen in Figure 4 above, a handheld 20 or 28 dioptre (unit used to measure power of lens) lens is used with an indirect ophthalmoscope, a kind of headgear mounted with a light, which the eye care professional can use to see and magnify the retina. A scleral depressor is a probe that is used to carefully indent the eye to be able to see the periphery of the retina.

To follow the appearance of the retina through time, pictures can be taken for your eye care professional to compare between visits. These include standard photography of the retina or scans like optical coherence tomography (OCT). An OCT allows the eye care professional to analyse the different layers of the retina and to check whether there are new CNV to be treated.
Complications of myopia macular degeneration
Multiple complications can occur from MMD [2].
First, the back of the eye is more likely to stretch further and create a protrusion called a posterior staphyloma.
Second, there can be new blood vessels that grow beneath and into the retina where they should not be. This can grow into membranes in the macular. These are called choroidal neovascularization (CNV) or choroidal neovascular membranes.
Third, the stretching can cause cracks to occur in the retina called lacquer cracks. On its own they do not cause much trouble, but over time, they accelerate the loss of retinal layers.
Fourth, there can be traction between the vitreous and the macular, causing something called myopic traction maculopathy which pulls at the centre of vision, putting the patient at risk for vision loss.
Is there a treatment for macular degeneration?
There are no known treatments to slow down the progression of the retinal atrophy and stretching of the eye for now, including the posterior staphyloma and lacquer cracks. There are however multiple treatments for other complications caused by myopia.
If there are retinal tears or holes, an ophthalmologist who is a medical doctor specialized in eye health can offer a short procedure called a laser retinopexy. That is when the ophthalmologist uses a laser to solidify the retina around the tear to prevent the vitreous from going behind the tear or hole and detaching the retina.
If the retina detaches because of a tear or hole, an ophthalmologist specialized in vitreous and retinal surgeries will offer you an operation to reattach the retina. A similar operation can be offered if you have myopic tractional maculopathy. It allows the surgeon to remove the pulling of the macular by the vitreous and reduce the risk of complications and possibly improve vision [10].
For CNV, an ophthalmologist can offer an intravitreal injection of anti-vascular endothelial growth factor (anti-VEGF). The medication is injected directly in the eye after administration of numbing drops. This medication reduces the growth of new abnormal vessels and helps to improve vision [11].
Can myopic macular degeneration be prevented?
Unfortunately, there are no treatments to prevent myopic macular degeneration for now. However, regular annual examinations with an eye professional can help catch complications and treat them early.
To improve vision, it is important to remember to update your prescription of eyeglasses or contact lenses which can best correct vision. Talking to your eye care professional is important to find the best method for you. In patients who have decreasing vision, different aids and magnifying tools can be used to make it easier to function in day-to-day life. It is therefore important to talk about any difficulties with your eye care professional to get the most adapted help possible.
DISCLAIMER: THIS WEBSITE DOES NOT PROVIDE MEDICAL ADVICE
The information, including but not limited to, text, graphics, images and other material contained on this website are for informational purposes only. No material on this site is intended to be a substitute for professional medical advice, diagnosis or treatment. Always seek the advice of your physician or other qualified healthcare provider with any questions you may have regarding a medical condition or treatment and before undertaking a new healthcare regimen, and never disregard professional medical advice or delay in seeking it because of something you have read on this website.
References
- Y. Fang et al., “OCT-Based Diagnostic Criteria for Different Stages of Myopic Maculopathy,” Ophthalmology, vol. 126, no. 7, pp. 1018–1032, Jul. 2019, doi: 10.1016/j.ophtha.2019.01.012.
- A. P. Schachat, Ed., Ryan’s retina, Sixth edition. Edinburgh ; New York: Elsevier, 2018.
- J. Vongphanit, P. Mitchell, and J. J. Wang, “Prevalence and progression of myopic retinopathy in an older population,” Ophthalmology, vol. 109, no. 4, pp. 704–711, Apr. 2002, doi: 10.1016/S0161-6420(01)01024-7.
- H. H. Liu, L. Xu, Y. X. Wang, S. Wang, Q. S. You, and J. B. Jonas, “Prevalence and Progression of Myopic Retinopathy in Chinese Adults: The Beijing Eye Study,” Ophthalmology, vol. 117, no. 9, pp. 1763–1768, Sep. 2010, doi: 10.1016/j.ophtha.2010.01.020.
- E. Ueda et al., “Five-Year Incidence of Myopic Maculopathy in a General Japanese Population,” JAMA Ophthalmol, vol. 138, no. 8, pp. 1–7, Aug. 2020, doi: 10.1001/jamaophthalmol.2020.2211.
- M. Zou et al., “Prevalence of myopic macular degeneration worldwide: a systematic review and meta-analysis,” British Journal of Ophthalmology, vol. 104, no. 12, pp. 1748–1754, Dec. 2020, doi: 10.1136/bjophthalmol-2019-315298.
- Amy Dinardo and Philip Walling, “The Lost Arts of Optometry, Part Three: Going Back to Gonio,” Review of Optometry. https://www.reviewofoptometry.com/article/the-lost-arts-of-optometry-part-three-going-back-to-gonio-44408 (accessed Aug. 25, 2021).
- Christopher Nathaniel Roybal, “Indirect Ophthalmoscopy 101,” American Academy of Ophthalmology, May 15, 2017. https://www.aao.org/young-ophthalmologists/yo-info/article/indirect-ophthalmoscopy-101 (accessed Aug. 25, 2021).
- Retina Macula Institute, “Ocular Ultrasound,” Retina Macula Institute. https://retinamaculainstitute.com/ocular-ultrasound (accessed Aug. 25, 2021).
- N. Shimada, Y. Sugamoto, M. Ogawa, H. Takase, and K. Ohno-Matsui, “Fovea-Sparing Internal Limiting Membrane Peeling for Myopic Traction Maculopathy,” American Journal of Ophthalmology, vol. 154, no. 4, pp. 693–701, Oct. 2012, doi: 10.1016/j.ajo.2012.04.013.
- C. M. G. Cheung et al., “Influence of myopic macular degeneration severity on treatment outcomes with intravitreal aflibercept in the MYRROR study,” Acta Ophthalmologica, vol. 97, no. 5, pp. e729–e735, 2019, doi: 10.1111/aos.14035.
Tools Designed for Healthier Eyes
Explore our specifically designed products and services backed by eye health professionals to help keep your children safe online and their eyes healthy.
