Fuchs’ Endothelial Dystrophy
Fuch’s endothelial dystrophy – Written by Dr. Philipp Roberts, MD, PhD and Dr. Elsie Chan, B.Sc(Med) Hons, MBBS(Hons), MPH, FRANZCO.
What is Fuchs’ endothelial dystrophy?
The cornea is the clear window on the front of the eye that focuses light and allows a person to see. The innermost layer of the cornea is called the endothelium. The endothelium is made up of a layer of endothelial cells that pump fluid out of the cornea, thereby keeping it clear. Fuchs’ endothelial dystrophy is a condition which affects the endothelium.
In the earliest stages, there is deposition of abnormal material on the endothelium (called ‘guttae’). This can cause reduced vision and glare as it interferes with the clarity of the cornea. This leads to loss of endothelial cell function and swelling of the cornea. This swelling causes reduced vision. In the most advanced cases, the cornea becomes so swollen that blisters (bullae) can form on the surface (epithelial layer) of the cornea leading to irritation and pain [1,2]. It is named after the ophthalmologist who first described the condition, Ernst Fuchs.
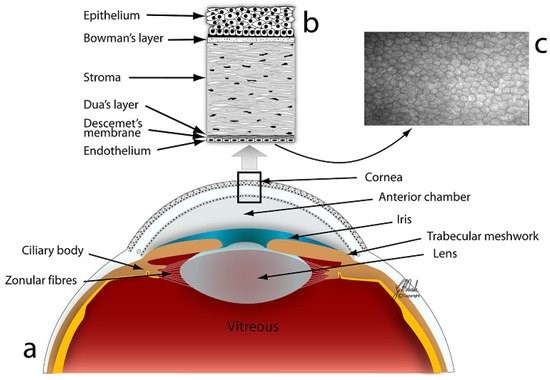
(c) microscopic image of the corneal endothelium (Source: J. Navaratnam et al.,”Substrates for Expansion of Corneal Endothelial Cells towards Bioengineering of Human Corneal Endothelium”, 2015)
The following sections will briefly outline why Fuch’s endothelial dystrophy develops, its signs and symptoms, and some insights into its management and treatment.
How common is Fuchs’ endothelial dystrophy?
Fuchs’ endothelial dystrophy is a very common condition, affecting between 3.7 to 11% of the population. It is more common in females than males [3]. It is one of the most common reasons for corneal transplantation worldwide.
Why causes Fuchs’ endothelial dystrophy?

Fuchs’ endothelial dystrophy is often inherited. Different genetic abnormalities have been implicated with the condition, but an exact gene has not been identified. Other factors that may influence the onset of the disease are environmental factors such as smoking, ultraviolet light exposure and diabetes.
What are the signs and symptoms of Fuchs’ endothelial dystrophy?
Most people with Fuchs’ endothelial dystrophy develop symptoms when they reach their 40s or 50s. However, there is a group of people who develop symptoms in their 20s or earlier.
Symptoms of Fuch’s endothelial dystrophy
Early stages
- Blurred vision
- Caused by the guttae, with or without swelling of the cornea.
- It may be worse in the morning and improve throughout the day. The reduced vision in the morning is due to fluid accumulating in the cornea overnight when the eyelids are closed. When the eyelids are open during the day, the cornea dries as it is exposed to the air, and the vision improves.
- Light sensitivity
Late stages (when bullae, or blisters, develop)
- Pain
- Redness
- Irritation
- Tearing
Signs of Fuch’s endothelial dystrophy
Fuchs’ endothelial dystrophy is diagnosed based on a comprehensive eye examination by an eye health professional. A specialised microscope called a slit lamp is used to examine the cornea in detail. The signs that are seen include:
- Guttae
- Swelling of the cornea
- Blisters (bullae) on the surface layer of the cornea
If you experience any of these signs and symptoms, schedule an appointment with an eye health professional to get your eyes checked. It is also important to note that the development of eye conditions may even start before symptoms appear, which makes going for regular and timely eye checks that much more essential.
Does Fuchs’ endothelial dystrophy get worse with time?
Fuchs’ endothelial dystrophy gradually worsens with age but often only very slowly.

How is Fuchs’ endothelial dystrophy diagnosed?
Fuchs’ endothelial dystrophy is diagnosed by an eye health professional based on routine questions and a comprehensive eye exam. Using a slit lamp, the eye health professional can look for the changes typical of Fuchs’ endothelial dystrophy (e.g. guttae with, or without corneal swelling).

To help detect early stages of corneal swelling, different machines can be used to measure the thickness of the cornea. This can be useful to monitor the condition over time but is not essential.
A different type of microscope (specular microscope) with high magnification can also be used to take an image of the endothelial cell layer. This allows direct imaging of the guttae, and of the number, size and shape of the endothelial cells (Figure 4).
How is Fuchs’ endothelial dystrophy treated?
There are non-surgical and surgical treatment options that can be offered.
Non-surgical treatment
Non-surgical treatment will only improve the symptoms in the short term, but do not reverse the underlying problem. Using a hairdryer to dry the cornea in the morning can be helpful to improve vision. This needs to be repeated every morning since the cornea will become swollen again overnight. Another option is the use of special eye drops containing a high concentration of salt, which also helps to dry the cornea.
There are ongoing studies with eye drops that may improve endothelial cell function. These eye drops, however, are not yet approved for Fuchs’ endothelial dystrophy and are still under investigation [4].
Surgical treatment
The main treatment for Fuchs’ endothelial dystrophy is corneal transplantation surgery to replace the abnormal endothelial layer of the cornea with a thin layer from a donor cornea. While there are risks of surgery, such as rejection, failure of the transplant over time and raised eye (intraocular) pressure, the success rate is high.
Future treatments
Newer surgical treatments without the need for a corneal transplant are currently being investigated in clinical studies. Other treatments under early investigation include gene therapy, which may reduce the need for surgery.
What can I do if I have been diagnosed with Fuchs’ endothelial dystrophy?
There are no preventative measures you can take to stop the condition from worsening. Regular eye check ups are recommended to monitor your vision and eye health. If your necessary, you will be offered treatment by the eye health professional.
DISCLAIMER: THIS WEBSITE DOES NOT PROVIDE MEDICAL ADVICE
The information, including but not limited to, text, graphics, images and other material contained on this website are for informational purposes only. No material on this site is intended to be a substitute for professional medical advice, diagnosis or treatment. Always seek the advice of your physician or other qualified healthcare provider with any questions you may have regarding a medical condition or treatment and before undertaking a new healthcare regimen, and never disregard professional medical advice or delay in seeking it because of something you have read on this website.
References:
- S. Weiss, H. U. Moller and A. J. Aldave et al., “IC3D classification of corneal dystrophies – edition 2,” Cornea, vol. 34, no. 2, pp. 117-159, 2015.
- A. Matthaei et al., “Fuchs endothelial corneal dystrophy: clinical, genetic, pathophysiologic, and therapeutic aspects,” Annu Rev Vis Sci, vol. 5, no. 1, pp. 151-175, 2019 Sep, doi: 10.1146/annurev-vision-091718-014852.
- O. Tone et al., “Fuchs endothelial corneal dystrophy: the viscious cycle of Fuchs pathogenesis,” Prog Retin Eye Res, vol. 80, pp. 100863, 2021 Jan, doi: 10.1016/j.preteyeres.2020.100863.
- A. Syed and C. J. Rapuano, “Rho kinase (ROCK) inhibitors in the management of corneal endothelial disease,” Curr Opin Ophthalmol, vol. 32, no. 3, pp. 268-274, 2021 May, doi : 10.1097/ICU.0000000000000748.
Tools Designed for Healthier Eyes
Explore our specifically designed products and services backed by eye health professionals to help keep your children safe online and their eyes healthy.
